WASHINGTON D.C. — In a development that could signal the beginning of the end for chronic joint pain, researchers funded by the federal Advanced Research Projects Agency for Health (ARPA-H) have successfully engineered functional, lab-grown cartilage. This breakthrough, announced Tuesday, offers a potential “holy grail” for the more than 32 million Americans currently living with the debilitating effects of osteoarthritis.
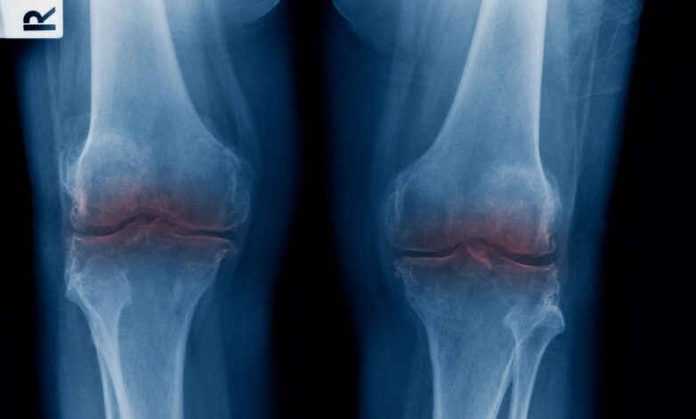
For decades, the medical community has struggled with a fundamental biological hurdle: human cartilage, the slippery tissue that cushions joints, does not heal itself. Unlike skin or bone, it lacks its own blood supply. Once it wears away due to age, injury, or disease, it is gone for good—leaving patients to endure bone-on-bone friction that leads to agonizing pain and, eventually, invasive joint replacement surgery.
However, this new study suggests that the biological “dead end” of cartilage repair may finally have been bypassed. Utilizing a sophisticated blend of a patient’s own stem cells and a bio-synthetic “scaffold,” scientists have demonstrated the ability to grow new, durable tissue that mimics the mechanical properties of natural cartilage.
The study, which was initially conducted in large animal models, showed that the lab-grown tissue integrated seamlessly with the surrounding bone. Within weeks, the subjects regained full range of motion. Most significantly, the engineered cartilage did not degrade under the stress of weight-bearing movement—a common failure point in previous experimental treatments.
“We aren’t just patching a hole; we are restoring the joint’s original architecture,” said one of the lead researchers during the unveiling in Washington. “This isn’t a temporary filler. This is living tissue that grows and adapts with the patient. It represents a paradigm shift from managing pain to actually curing the underlying structural damage.”
The implications for public health are staggering. Osteoarthritis is a leading cause of disability worldwide, costing the U.S. economy billions of dollars annually in lost productivity and healthcare expenses. Current solutions, such as cortisone shots or physical therapy, offer only temporary relief. Even total knee or hip replacements, while effective, are major surgeries with long recovery times and a finite lifespan of 15 to 20 years.
For younger patients or athletes who suffer joint injuries, this breakthrough could mean returning to peak performance without the looming shadow of early-onset arthritis. For the elderly, it could mean maintaining independence and mobility well into their sunset years.
The next step is the most critical: human clinical trials. ARPA-H officials confirmed today that they are fast-tracking the regulatory process to begin testing in human volunteers within the next eighteen months. If these trials mirror the success seen in the laboratory, the procedure could be widely available at specialized orthopedic centers by the end of the decade.
While the researchers cautioned that widespread availability is still several years away, the mood at the announcement was one of cautious triumph. The technology behind the “scaffold”—a 3D-printed lattice that eventually dissolves once the new cartilage takes hold—is being hailed as a masterpiece of bio-engineering.
As the global population ages, the demand for joint-related care is expected to skyrocket. This American-led breakthrough offers a vision of a future where “getting older” no longer automatically means “slowing down.” For millions of people currently dreading their next staircase or morning walk, the news from Washington is more than just a scientific update—it is a promise of a life reclaimed from pain.