BALTIMORE, MD — For decades, the medical community has grappled with a frustrating paradox: the human liver is one of the body’s most resilient organs, capable of incredible regeneration, yet it is also one of the most stoic. It rarely complains until it is too late. By the time symptoms of cirrhosis or liver cancer appear, the damage is often irreversible.
But as of March 2026, that era of medical “guesswork” is coming to a definitive end. A groundbreaking AI-driven “liquid biopsy” has officially cleared clinical hurdles and begun its rollout across major U.S. hospital systems, promising to catch liver disease not just months, but years before it becomes life-threatening.
Cracking the Genetic Code
The technology, developed through a massive collaborative effort between researchers at Johns Hopkins and AI specialists in Silicon Valley, operates on a microscopic scale. Every day, our cells shed tiny fragments of DNA into our bloodstream. When an organ is under stress—even at a level invisible to traditional scans—the patterns of these DNA fragments change.
The new AI tool, dubbed “HepaScan AI,” uses deep-learning algorithms to recognize these “molecular signatures” of early-stage fibrosis. In trials involving over 15,000 patients, the test demonstrated a 94% accuracy rate in identifying Stage 1 liver scarring—a phase where the condition can often be entirely reversed through simple lifestyle changes or newly developed targeted therapies.
“We are moving from a reactive ‘wait-and-see’ model of medicine to a proactive ‘detect-and-defend’ model,” says Dr. Aris Thorp, a leading hepatologist involved in the rollout. “For the millions of Americans living with undiagnosed fatty liver disease, this test is quite literally a lifesaver.”
A Ripple Effect for Public Health
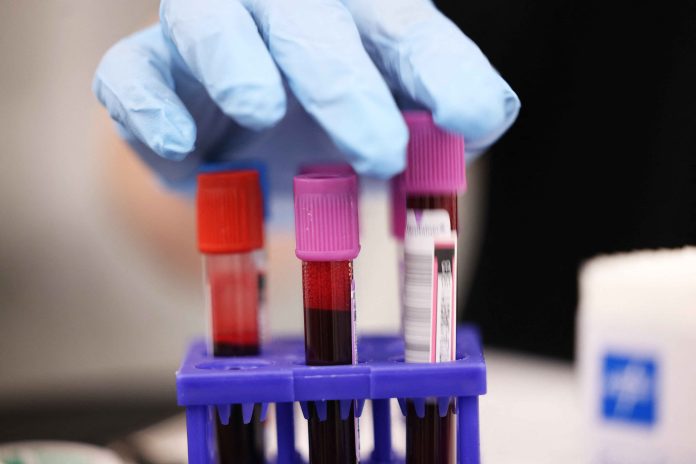
The timing of this breakthrough is critical. With the rise of metabolic-associated fatty liver disease (MASLD), health experts had feared a looming “transplant crisis.” The AI liquid biopsy offers a way to flatten that curve. Because the test requires only a standard blood draw, it can be integrated into annual physical exams, making high-level diagnostic power accessible to rural clinics and underserved urban centers alike.
The success of the liver test is also acting as a “North Star” for other fields. Researchers are already using the same AI framework to develop similar early-warning tests for pancreatic and ovarian cancers—diseases that have historically been difficult to screen in their early stages.
The Power of Prevention
For patients, the impact is personal. Take the case of 42-year-old Maryland resident Marcus Thorne, one of the first to receive the test during its pilot phase. “I felt perfectly fine,” Thorne says. “But the scan showed my liver was under early stress. Because we caught it now, I changed my diet and started a mild medication. A year from now, I might have been looking at a much scarier conversation. Today, I’m just looking at a healthy future.”
As this technology becomes a standard of care in 2026, the “silent killer” is finally losing its voice. In its place is a new narrative of hope, where the most dangerous diseases are the ones we simply stop before they ever truly begin.















